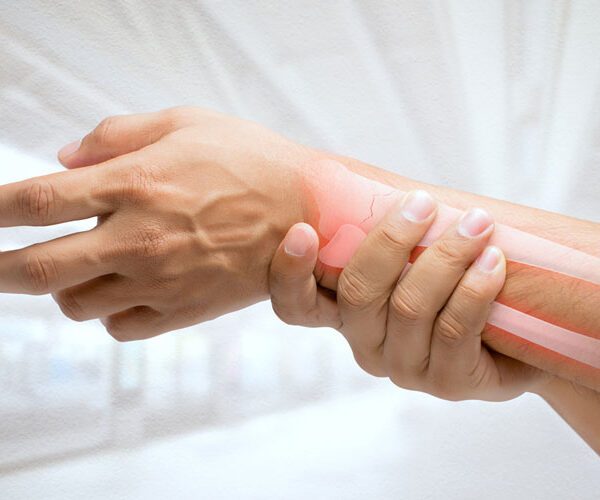
Bone loss due to osteoporosis takes place without symptoms, making bones more fragile and escaping detection until bones become weak and fracture. Fractures can be debilitating, life-changing injuries, but many people don’t connect their broken bones with osteoporosis. For those who have broken a bone, recovery is the topmost priority. But determining whether a fracture is a symptom of osteoporosis is equally important.
That’s because people with osteoporosis are at higher risk for future fractures. And for those over 50, the likelihood is very high that osteoporosis was a contributing factor to the first fracture. To prevent the next one, it’s critical to act quickly after a fracture to evaluate for osteoporosis, educate about strengthening bones, and employ strategies to reduce the risk of falling.
Evaluating for Osteoporosis After a Fracture
Over 53 million people in the US are either at high risk (due to osteopenia) or already have osteoporosis. The U.S. Preventive Services Task Force (USPSTF) recommends screening for osteoporosis in women aged 65 years and older and in women younger than age 65 years who have been through menopause and are at increased risk for osteoporosis. But osteoporosis is underdiagnosed due to low adherence to screening recommendations.
Most hip, spine, and wrist fractures are attributable to osteoporosis, but surprisingly, many patients are never seen for an osteoporosis evaluation or treatment after the initial fracture. Evaluating factors such as medical history, lifestyle, family history of fractures, hormone levels, use of medications that contribute to bone fragility, and the results of a bone mineral density test are the gold standard components of the osteoporosis evaluation.
Improving patient awareness of the link between an initial fracture and osteoporosis and incentivizing clinicians to perform recommended screening post-fracture can drive prevention efforts and interventions to lower the risk of morbidity and mortality related to osteoporotic fractures.
Educating Patients About Strengthening and Protecting Bones
Arming patients with the information they need to make informed decisions is the key to treatment adherence. Treatment strategies might include discussing medication or hormone replacement therapy (for men). Aside from medication, other strategies might include:
- Following a diet rich in Calcium and vitamin D, including supplementation if necessary
- Lowering sodium intake
- Adhering to recommended daily protein intake for men (56 grams) and women (46 grams)
- Quitting smoking
Patients are more receptive to recommendations when the clinician takes the time to understand their preferences, plainly explains the risks and benefits of treatment, creates an environment for shared decision making and frames advice around the factors they find important.
Preventing Falls
In an effort to avoid a repeat fracture, many people reduce or altogether eliminate their day-to-day level of physical activity and exercise. But in fact, this has the opposite effect. Instead, patients should be encouraged to continue being physically active, as exercise helps reduce the risk of fracture by preserving bones and by helping prevent falls in the following ways:
Weight-bearing (walking, stairs, dancing) and resistance (free weights or machine weights) exercise builds and maintains bone density, improving strength, balance, and flexibility, all of which reduce the chance of falls
Patients should also be encouraged to correct vision or hearing loss, as both are contributors to falls. Reviewing medications for potential interactions or effects that increase fall risk is also important. Finally, assessing the home environment for risks such as poor lighting (especially in the bedroom and bathroom), loose rugs or cords, or other tripping hazards is critical.
After the first fracture, patients should act fast to prevent the next one. Clinicians can help patients take charge of their health and wellbeing by pointing them to these additional resources:
NIH Osteoporosis and Related Bone Diseases ~ National Resource Center
https://www.bones.nih.gov
National Institute on Aging
https://www.nia.nih.gov
American Academy of Orthopaedic Surgeons
https://www.aaos.org
National Osteoporosis Foundation
https://www.nof.org